Skip NavigationSkip to Primary Content


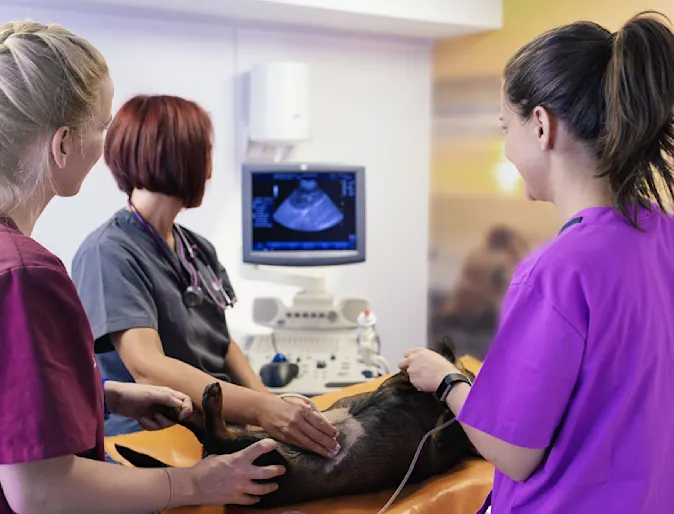
Advanced Imaging
Combined with our board-certified specialized procedures and skilled emergency veterinarians and technicians, ASECB is unmatched for the level of expertise and experience you need when your pet is ill.

Dentistry & Oral Surgery
Dr. Monica Morgado of Animal Specialty and Emergency Center of Brevard provides advanced dentistry and oral surgery to care for your pet's oral health.

Board Certified Canine Rehabilitation
Physical rehabilitation is also very beneficial to help maintain good function for patients with chronic neurological disorders, chronic arthritis, weight problems, or other musculoskeletal disorders.

You Can Count on Us
Whether your pet swallowed a fishhook, was attacked by another animal, or developed a life-threatening illness, our Pet Care Team is available 24 hours per day, 7 days per week to provide emergency care. Our specialist care is available by referral appointment only Monday through Friday 8:00 AM – 4:00 PM.
Call us immediately and speak to one of our experienced emergency team members so we can assess your situation and determine the best course of action. In the event your pet does need to visit our facility, an advance call also helps us respond to your medical needs more quickly when you arrive at the hospital.
Client Reviews & Testimonials
We value our clients’ experience at Animal Specialty & Emergency Center of Brevard. Here’s what some people are saying about us.
